[fusion_builder_container hundred_percent=”no” hundred_percent_height=”no” hundred_percent_height_scroll=”no” hundred_percent_height_center_content=”yes” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” status=”published” publish_date=”” class=”” id=”” link_color=”” link_hover_color=”” border_size=”” border_color=”” border_style=”solid” margin_top=”” margin_bottom=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” enable_mobile=”no” parallax_speed=”0.3″ background_blend_mode=”none” video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” video_preview_image=”” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″][fusion_builder_row][fusion_builder_column type=”1_6″ layout=”1_6″ spacing=”” center_content=”no” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” hover_type=”none” border_size=”0″ border_color=”” border_style=”solid” border_position=”all” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”” margin_bottom=”” background_type=”single” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_image_id=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”no”][/fusion_builder_column][fusion_builder_column type=”2_3″ layout=”2_3″ spacing=”” center_content=”no” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” hover_type=”none” border_size=”0″ border_color=”” border_style=”solid” border_position=”all” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”” margin_bottom=”” background_type=”single” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_image_id=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”no”][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Since July of 2020, the Institute for Solidarity in Asia (ISA) has been initiating the conversation with the key sectors of Philippine society through the #ISAngKilosBayan Advocacy Series, tackling critical strategies as well as the human and community side of responding to the COVID-19 pandemic.
The health sector-focused segment journeyed from the frontlines of Visayas and Mindanao, to that of Luzon, and recently concluded with the episode of the National Capital Region (NCR) — one of the regions hardest hit by the pandemic.
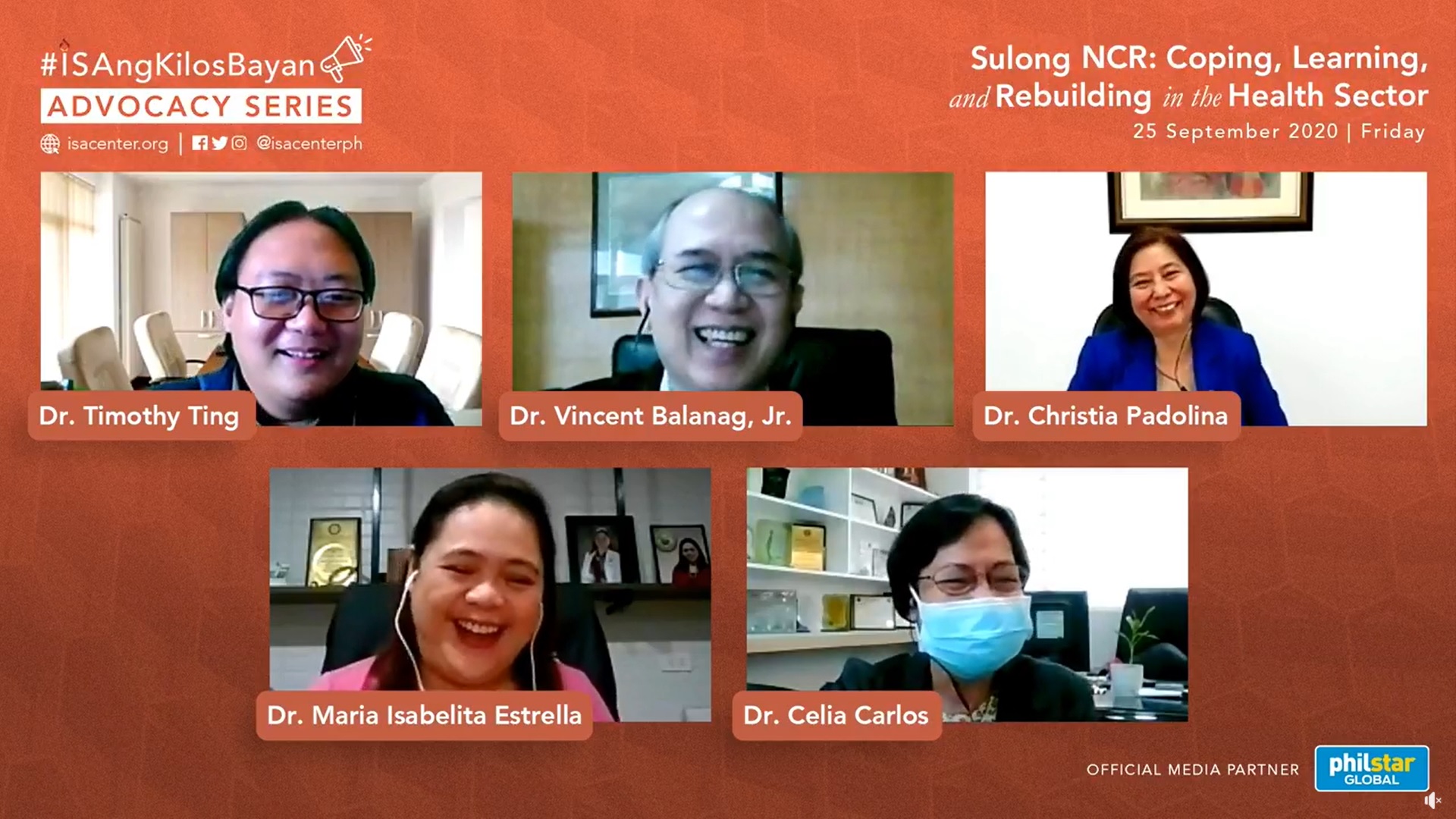
The Sulong NCR episode featured Dr. Vincent Balanag Jr., Executive Director of the Lung Center of the Philippines (LCP), Dr. Christia Padolina, Chief of the Navotas City Hospital (NCH), Dr. Maria Isabelita Maligaya-Estrella, Medical Center Chief II of Tondo Medical Center (TMC), and Dr. Celia Carlos, Director IV of the Research Institute for Tropical Medicine (RITM). To elevate the discussion further, ISA invited University of the Philippines Manila’s Department of Health Policy and Administration Chair, Dr. Carmelita Canila, as reactor, and Asian Institute of Management Adjunct Professor for the TeaM Energy Center for Bridging Leadership, Dr. Timothy Ting, as moderator.
[/fusion_text][fusion_imageframe image_id=”8950|full” max_width=”” style_type=”” blur=”” stylecolor=”” hover_type=”none” bordersize=”” bordercolor=”” borderradius=”” align=”none” lightbox=”no” gallery_id=”” lightbox_image=”” lightbox_image_id=”” alt=”” link=”” linktarget=”_self” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″]https://isacenter.org/wp-content/uploads/2020/09/Sulong-NCR-1.jpg[/fusion_imageframe][fusion_builder_row_inner][fusion_builder_column_inner type=”1_1″ layout=”1_1″ spacing=”” center_content=”no” hover_type=”none” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” border_size=”0″ border_color=”” border_style=”solid” border_position=”all” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” dimension_margin=”” background_type=”single” background_color=”” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_image=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”no” element_content=””][/fusion_builder_column_inner][/fusion_builder_row_inner][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Dealing with an overburdened system
At the onset of the panel discussion, the hospital leaders enumerated their unique experiences from when the pandemic was still in its early days.
For LCP, Dr. Balanag recounted how they already anticipated that the hospital was going to be heavily involved in the growing issue, seeing that COVID-19 was a respiratory virus.
“We [had been] involved in past pandemics such as SARS, H1N1, which in a way, prepared us for this incoming pandemic. We had existing policies for prevention and control. ” said the Executive Director.
When LCP soon became a COVID-19 referral center, the institution had to ask the Department of Health to support even the non-COVID functions of the hospital, as they were a specialty center for other complicated diseases.
Similarly, at TMC, Dr. Maligaya-Estrella shared how the right protocols were already in place when the pandemic came. However, they had great difficulty when many of their staff turned out COVID-positive and had to be admitted in the hospital.
“We were [feeling] so down. The fear was there [because] during the start of the pandemic, we were hearing that doctors and consultants were dying because of COVID,” said the Medical Center Chief.
This also added to the fact that TMC was situated at the heart of Balut, Tondo, where community transmission was high.
“A lot of our patients from Tondo were COVID-positive. When they came to us, they [already] had difficulty breathing—a lot of DOA (Dead on Arrival), ER deaths—that time was very difficult,” she shared.
Another area that had to deal with high community transmission was Navotas City. NCH Chief Dr. Padolina described the peak of the crisis, wherein the growing number of cases in the city overwhelmed their hospital.
“[Other healthcare facilities] are in the same boat as we are – [dealing with] problems of over-congestion and an overburdened healthcare system. There was an immediate need to ensure that the functions were cohesive. If we say [to patients that] the health centers couldn’t accommodate them, they would go to the hospitals, which will be bogged down with admissions because the tests were not coming early. We can’t transfer them because other hospitals are also filled up,” narrated the Chief.
Related to that, Dr. Carlos gave a glimpse into the labs of RITM, which for a long time, was the only COVID-19 testing center in the country.
“We were the only testing lab for COVID for almost 2.5 months and initially we had one lab in charge of that, but their capacity was limited to 300 to 400 [tests] a day. The samples were rapidly increasing so we had to adjust. From 300, we were able to increase to 2500 a day,” said Dr. Carlos.
On top of their testing function, RITM also had to validate testing kits, advise the DOH on COVID protocols, and certify other labs that were putting up COVID testing facilities. The latter, according to the Director, was not an easy task as COVID labs were unlike regular labs.
“We needed to make sure that the working areas are bio safe and that there would be no lab-acquired infections,” added Dr. Carlos.
[/fusion_text][fusion_imageframe image_id=”8949|full” max_width=”” style_type=”” blur=”” stylecolor=”” hover_type=”none” bordersize=”” bordercolor=”” borderradius=”” align=”none” lightbox=”no” gallery_id=”” lightbox_image=”” lightbox_image_id=”” alt=”” link=”” linktarget=”_self” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″]https://isacenter.org/wp-content/uploads/2020/09/Sulong-NCR-2.jpg[/fusion_imageframe][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
In photo: Panel discussion speakers tackle their experiences from their respective hospitals as they responded to COVID-19
[/fusion_text][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Weathering through the crisis
Throughout implementing new protocols and initiatives, the NCR hospital leaders gathered critical learnings that helped them weather through the crisis.
Serving as both the NCH Chief and Navotas City Health Officer, Dr. Padolina expressed how the biggest learning she had was on trusting and delegating some of the major activities they had to undertake in crisis response so that she could look at the bigger picture. This approach allowed her to engage with the LGU-side stakeholders who could bring in information and carry out interventions at the community level while keeping in sync with the local health department.
She also added the importance of empowering the hospital staff to devise innovative ways to make their areas safe from COVID.
“We had to be self-sufficient. We cannot transfer patients all at the same time. Even if [their area] wasn’t designed to address COVID patients, we had to adjust and innovate so we can create COVID-safe areas,” said Dr. Padolina.
As the institute for dealing with major health phenomena in the country, the learnings from RITM were on a much wider scale.
“Our country needs to do a lot more in preparing for a health event,” said Dr. Carlos.
Though she acknowledges that the Philippines has a good system for disaster response, Dr. Carlos maintains that biological events such as infectious diseases should also be covered through an action plan. In her view, the next step that must follow is the high level endorsement, i.e. a law to concretize the national action plan sooner.
“There are now a lot of bills in the senate and congress [and] RITM attends all of these [sessions] to input our suggestions. Eventually, these bills, when implemented, can make a big difference for our country’s response in case there is another similar pandemic in the future.
[/fusion_text][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Future-proofing the health system
Indeed, the new normal as a result this pandemic seems to be the topic at hand for many sectors and individuals. This was what reactor Dr. Canila gave her input on as the discussion came to a close.
“We need to move towards future-proofing our health system. How do we do that? All our hospital leaders have pinpointed the way forward,” began Dr. Canila.
The first area that was crucial, according to her, was safeguarding the health workers and their families. In addressing this issue, Dr. Canila emphasized the need to be more compassionate “people managers”.
“We’re not only managing the facilities and the local health system. Foremost [in] our job is that we are people managers,” said the UPM Department of Health Policy and Administration Chair.
[/fusion_text][fusion_imageframe image_id=”8948|full” max_width=”” style_type=”” blur=”” stylecolor=”” hover_type=”none” bordersize=”” bordercolor=”” borderradius=”” align=”none” lightbox=”no” gallery_id=”” lightbox_image=”” lightbox_image_id=”” alt=”” link=”” linktarget=”_self” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″]https://isacenter.org/wp-content/uploads/2020/09/Sulong-NCR-3.jpg[/fusion_imageframe][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
In photo: Dr. Carmelita Canila provides her input on the emerging healthcare system as a result of this pandemic
[/fusion_text][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
On that note, she also mentioned that the challenge now for leaders is to practice Adaptive Leadership.
“[Because of COVID-19,] government institutions were thrust to the limelight to become learning organizations very fast. There’s a need to be adaptive, to cope, and to be better informed by data. These data comes from not only institutions but also communities,” stated Dr. Canila. Through this connection between institutions and communities, she said, we can realize the impact of combining the whole of government approach and the whole of people approach.
Finally, she underscored the importance of the Stewardship Role of government.
“If we have packets of facilities that have shown their governance structures, there is a need for government structure to support these facilities because they cannot move forward without the stewardship of the national government. The national government has to rethink how it can proactively support the local health system based on the current experiences. We cannot wait because [hospitals] deal with death and emotions and families,” advised Dr. Canila.
To close the discussion, Dr. Canila expressed that this way forward also calls on a great deal of rewriting on everyone’s part — not just of the old standards of operating, but also the cultural practices we had grown accustomed to. For instance, part of the culture within hospitals and workplaces in general is having moments of celebration together with food-sharing.
“These are the things that make our work lively [that we can no longer do] but we [still] need to find ways to celebrate in our institutions. We need to rewrite our cultural practices and it will take a while,” she said.
Many learnings and innovations have emerged from this crisis. It is now up to the different sectors of society to work together towards building for a better future for our Dream Philippines.
[/fusion_text][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
View the full episodes of the #ISAngKilosBayan Advocacy Series here.
Check out the highlights from the other episodes here.
[/fusion_text][/fusion_builder_column][fusion_builder_column type=”1_6″ layout=”1_6″ spacing=”” center_content=”no” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” hover_type=”none” border_size=”0″ border_color=”” border_style=”solid” border_position=”all” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”” margin_bottom=”” background_type=”single” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_image_id=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”no”][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]